
A single nanoparticle does two jobs: enhancing the effectiveness of chemotherapy and reinvigorating the immune system.
Researchers at Tel Aviv University proved the efficacy of a cancer treatment that can overcome resistance to both chemotherapy and immunotherapy, according to a study published in late January in the journal Advanced Materials.
The study was led by TAU Vice President for Research and Development Professor Dan Peer, head of the Laboratory of Precision Nanomedicine at the Shmunis School of Biomedicine and Cancer Research, as well as Dr. Seok-Beom Yong of South Korea.
Chemo-immunotherapy, a combination of chemotherapy and immunotherapy, is considered the most advanced standard of care for various types of cancer. “This is the first instance of a single drug based on an RNA-loaded nanoparticle doing two very different, even opposite jobs,” explained Prof. Peer. “This is only an initial study, but it has enormous potential in the ongoing fight against cancer.” The two treatment types work in concert; chemotherapy destroys cancer cells while immunotherapy encourages the patient’s own immune system to also attack cancer cells.
Unfortunately, many patients respond poorly to this dual treatment because its targets are not specific enough.
“Chemo-resistant tumors pose a significant challenge in our endless battle against cancer,” said Prof. Peer. “We aim to silence the enzyme HO1 which enables tumors to develop resistance to chemotherapy and to conceal themselves from the immune system. But existing methods for silencing HO1 resemble using an F-16 fighter jet to blast a tiny ant.”
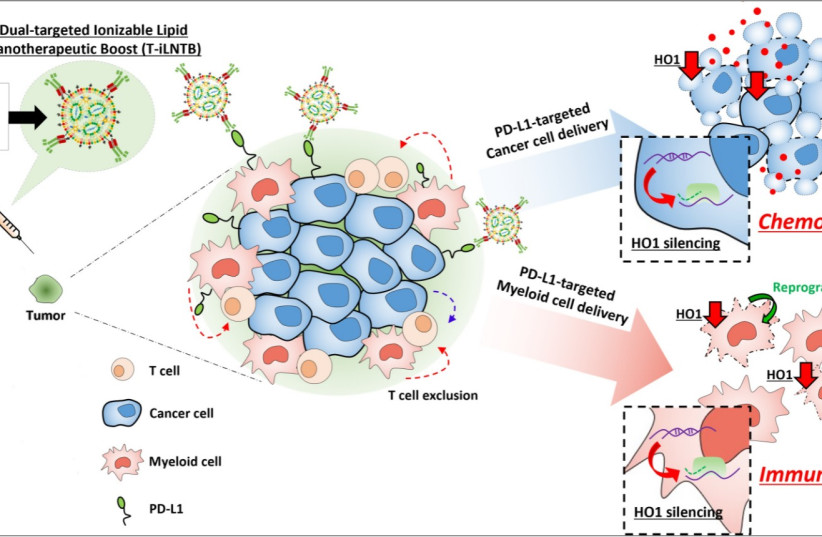

The TAU team is the first in the world to prove the viability of a drug delivery system based on lipid nanoparticles that target extremely specific cells – cancer cells for chemotherapy and immune cells for immunotherapy. Prof. Peer explained that “our new nanodrug knows how to precisely target the cancer cells, silence the enzyme, and expose the tumor to chemotherapy, without causing any damage to surrounding healthy cells. Afterward, the same nanoparticle goes on to the T-cells of the immune system and reprograms them to identify cancer cells.”
Funding for the study came from an European Research Council (ERC) grant from the European Union and a research scholarship from the South Korean government.
Source: JPOST